
Managing asthma to give you
freedom to enjoy life
Living with asthma means juggling all the factors that can make you or your child feel better or worse, or trigger an attack. Weather, exercise and even food can all impact asthma conditions. However, taking your asthma medication correctly, and following your treatment plan, can help you better manage day-to-day triggers and keep your asthma in control.
Asthma management products can help:

Reduce chronic asthma symptoms

Stay on track with your long-term treatment plan

Respond to triggers around you
Are you in control of your asthma?
If you think your or your child’s asthma is in control, you are in good company. Most people living with asthma believe they have their asthma under control, but studies have found that fewer than half of them actually do1. Read more on effective asthma management and the tools you can use to improve the quality of life for you or your child.
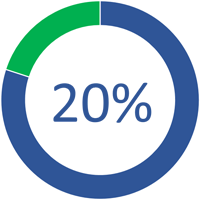
Less than 1 in every 5 Australians with asthma aged over 15 years have a written asthma action plan2.
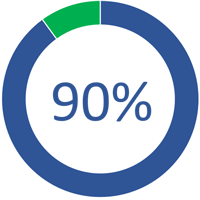
90% of patients have incorrect MDI technique3.
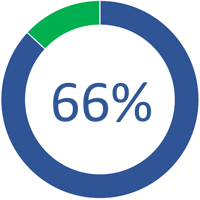
66% of individuals were identified with low adherence to prescribed medication4.

Nearly 1 in 3 adults miss at least 1 day of work each year because of their asthma5.

Nearly 1 in 2 children miss at least 1 day of school each year because of their asthma5.
Are you caring for a child with asthma?
Making sure your child is staying on track with his or her asthma treatment can be scary and stressful. Using medication delivery devices like an inhaler spacer or nebuliser can help your child get their medication to their lungs where it works and give you more peace of mind.



Breathing treatment wherever you are
Managing asthma can take commitment, but it doesn't have to tie you down or disrupt the daily routines of your life. There is a range of breathing treatments or nebulisers that gives you the flexibility to treat and manage your asthma at home, at school, or on the go. You can always choose the device that matches your lifestyle and routine!

Breathing treatment at home

Portable breathing treatment

Ask your healthcare professional or pharmacist about asthma management
Your healthcare professional or pharmacist can be a valuable resource for understanding the use and benefit of including asthma management devices as part of a treatment plan.
Frequently asked questions

Sign up to for more information from Philips

Are you a healthcare professional?
DISCLAIMER:
Information on this website is informational only and should not replace the advice of a physician.
ALWAYS FOLLOW THE DIRECTIONS FOR USE.
References: [1] gsk.com. Media/620439/the state-of-uncontrolled-asthma-in-america-infographic.pdf. Accessed October 2017. [2] Australian Government Productivity Commission (AGPC) 2018, Report on Government Services [3] Bidwal M, Lor K, Yu J, IpE. Evaluation of asthma medication adherence rates and strategies to improve adherence in the underserved population at a federally qualified health center. Res Social Adm Pharm. 2017, 13(4): 759-766. [4] Bonds R.S. Misuse of medical devices among patients in a tertiary care Allergy/Immunology practice. Journal of Allergy and Clinical Immunology, 2017, 133(3) supplement: AB156. [5] CDC National Asthma Control Program. Asthma’s Impact on the Nation. Accessed December 2016.
