Cultural change can be the hardest part of digital transformation in healthcare. To successfully drive this change, healthcare leaders need to have clarity of purpose, empower their people through ongoing training and education, and adopt more agile ways of working for continuous improvement.
Here’s a common fallacy I encounter during discussions on digital transformation. Let’s say you have something analog – for example, a paper patient record – and turn it into an electronic format. If you keep doing everything you used to do on paper, but now digitally, that’s not digital transformation. That’s simply digitizing an existing process. True digital transformation goes a step further: it reimagines what the healthcare experience could be for both patients and providers using digital technologies – which may involve entirely new processes and ways of working.
Returning to the paper chart example above, simply digitizing a paper record would miss the opportunity to integrate data from the patient’s electronic health record with other information sources – such as imaging studies, pathology data, genomic analysis, and patient reported data – to generate insights at scale. The impact of integrating information from various digital sources is easily seen at multidisciplinary tumor board meetings, where clinicians can review the longitudinal patient record at a glance. In a study conducted by Philips together with our innovation partner Karolinska University Hospital in Sweden, we demonstrated improved clinician experience in discussing complex tumor board cases, while reducing the overall time needed to discuss the materials for each case by 24% [1]. That’s digital transformation – a better experience with reduced operational friction.
Since digital transformation goes beyond simple digitization of current processes, the journey is non-trivial. As I discussed in a previous post, hospitals need secure and interoperable digital platforms to liberate data from silos and make it flow more freely. Yet technology is only part of the solution. Healthcare professionals need the right skills to feel confident and competent using new digital technologies. Different teams need to be on board with new, cross-functional ways of working.
It’s these human and cultural aspects of digital transformation that can make or break its success. Case in point, in a 2020 survey by Bain & Company, only 1% of healthcare executives said their digital investments had fully delivered on their expectations [2]. It led the authors to recommend that leaders make change management as much a priority as the technological aspects of digital transformation. I certainly agree with that! Digital transformation is about people, processes, and platforms – in that order.
So, what can healthcare leaders do to bring their physicians and staff along on this journey? Based on my experience spearheading innovation at various organizations, I see successful digital transformation in healthcare being driven by four cultural tenets.
1. Define your purpose close to where the transformation occurs
First, digital transformation in healthcare should be guided by a clear purpose articulated in a way that everyone in your organization can relate to. That means it needs to be concrete, practical, and specific. It should speak to the daily reality of physicians, nurses, and patients, and evoke strong mental images of how digital technology will change their lives for the better.
At its essence, I believe digital transformation is about removing friction from experiences. That’s how digital technology has transformed every aspect of our lives, from how we buy and how we communicate to how we get from A to B. When I’m driving to work and my car alerts me that I’m running low on gas while pointing me to the nearest gas station through an intelligent wayfinding app, that’s a frictionless experience. It has only been made possible through the relentless pursuit of simplification, taking out manual steps from what used to be a more cumbersome process, and combining data from multiple sources.
Digital transformation in healthcare should be guided by the same principle. When I was Chief Digital Officer at a large health system, physicians were consistently telling me that they spent too much time clicking their way through computer applications, at the expense of interacting with patients. Reducing the number of clicks became the driving purpose behind everything we did – whether it was in the way we employed our electronic medical record system, or in new scheduling applications that removed friction for our patients. In fact, I used to introduce myself and our team as ‘click reductionists’.
It’s a purpose that resonated widely and secured engagement from different teams because it was concrete, practical, and specific. Everyone could relate to it. Had we formulated it in loftier and more abstract terms, I doubt it would have been as effective. The closer you are able to define your purpose to where you actually want the transformation to occur, the more impactful it will be.

2. Empower your people through ongoing training and education
Next to a clear shared purpose, people also need the skills and competencies to adopt new, digitally transformed ways of working. With today’s pace of technological change, it can be easy to overlook the demands that those frequent changes place on people using the technology. Compounding the challenge is that medical education tends to trail behind technological advances, leaving many healthcare professionals underprepared for digitally enabled care delivery. As nurse entrepreneur Rebecca Love aptly put it in a report by EIT Health and McKinsey: “We spent more time learning how to make a bed than being prepared to use digital hospital systems” [3].
Education is therefore essential. Empowering healthcare professionals to be digitally competent requires a culture of continuous learning and development. That starts in medical or nursing school, where curricula should prioritize developing digital literacy, but it extends to day-to-day practice in hospitals.
For example, when Canadian healthcare provider Mackenzie Health set out to develop Canada’s first smart hospital, they realized how important it was to equip their staff with the necessary skills. As part of their 18-year strategic partnership with Philips, we helped them develop an integrated training program covering different hospital sites and equipment vendors. Pivotal to the success of such programs has been the involvement of ‘super users’, as part of a train-the-trainer concept. These super users continue to train current and incoming staff to proficiently operate systems, and they serve as internal champions who spearhead new ways of working [4].
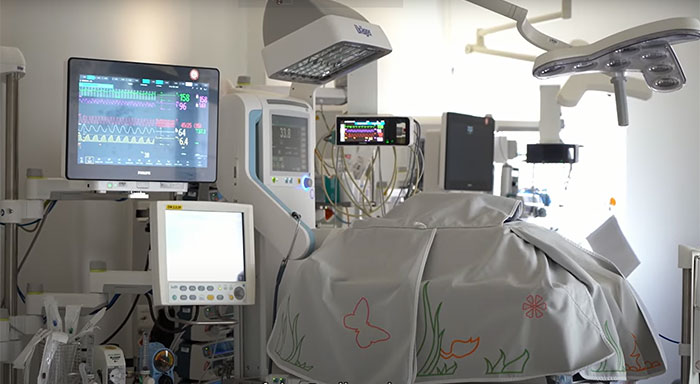
Beyond training and education, involving staff from an early stage – and bringing them physically together in the same room – also goes a long way towards adopting new ways of working. The video below shows a fantastic example. It tells the story of the Neonatal Intensive Care Unit (NICU) of Radboudumc Amalia Children’s Hospital in the Netherlands as it transitioned from open-floor nursing to single-bed units. Using a smart alarm system, staff are now alerted on care phones when sick or preterm babies are in need of specific attention. Delegates from each NICU function group joined co-creation sessions facilitated by Philips to shape new work processes together. The team was also consulted to set the right alarm thresholds to help reduce alarm fatigue. This helped to motivate and empower different function groups in the NICU to embrace the new ways of working.
3. Create a culture of experimentation and continuous optimization
Even with a compelling purpose and with people who are empowered to act on that purpose, there is no way of knowing beforehand what exactly the optimal outcomes of digital transformation will be or how to get there. There’s no perfect roadmap. But you don’t need one either. The trick is to re-route at every step of the journey, based on what you learn along the way.
That’s why experimentation is another key cultural driver of digital transformation. In healthcare, we like to believe that a new solution is not good enough for anyone until it’s good enough for everyone. But aiming for initial perfection is the antithesis of innovation. No digital solution can address the needs of every possible use case. By experimenting with new solutions on a small scale first – in a safe and controlled manner – and then refining them, you have a much better chance of ultimately driving large-scale transformation. Progress beats perfection because it allows you to learn and adjust.
That also requires rethinking traditional annual budgeting and multi-year planning cycles, which tend to slow down innovation in healthcare. Instead, lean funding and agile governance models allow innovation teams to experiment faster and then double down on what works. Coupled with the flexibility and scalability of cloud-based platforms, such agile ways of working enable innovation teams to put new digital applications into the hands of providers and patients more quickly, and then add new or improved features as they gather additional user feedback.
Plus, there’s another benefit to such an agile approach. By testing digital innovations with users in small increments, you’re also generating the familiarity and evidence that is needed to build trust with healthcare professionals.
Trust in digital health technology is a big deal, particularly as we head into the era of predictive AI. In fact, lack of trust has been a major barrier to clinical adoption of AI so far [5], for understandable reasons. If you’re a radiologist using AI algorithms to help identify potentially malignant tumors, you want to be sure you’re getting the right recommendations. Co-creation and rigorous validation with healthcare professionals can help build the trust and cultural willingness that is needed to ultimately embed such algorithms into the day-to-day workflow [6].
4. Consider new partnership models to optimize outcomes together
Much of what I have outlined here is not so much about the what of innovation – it’s about the how. That means healthcare leaders are also rethinking their relationships with technology partners like Philips. Technology has become table stakes. What customers are consistently telling us is that they are looking for a strategic partner who is in it for the long haul to have measurable impact on patient care together. Which brings me to my fourth and final cultural tenet: true digital transformation requires a new form of partnership. One with a shared focus on improving outcomes.
Patient monitoring is a great example. Traditionally, hospitals purchased monitors once every few years, after which they were responsible for the ongoing maintenance, operations, security and upgrades across their network. But that transactional model is ripe for disruption. Forward-looking healthcare providers such as Jackson Memorial Hospital in the US, have embraced a new model: Enterprise Monitoring as a Service (EMaaS). As part of this shared-risk, use-driven business model, Philips specialists work together with Jackson’s clinical and technical teams to address the hospital’s clinical, operational, and financial needs through ongoing workflow optimization, training and education, asset management, and data analytics for continuous improvement.
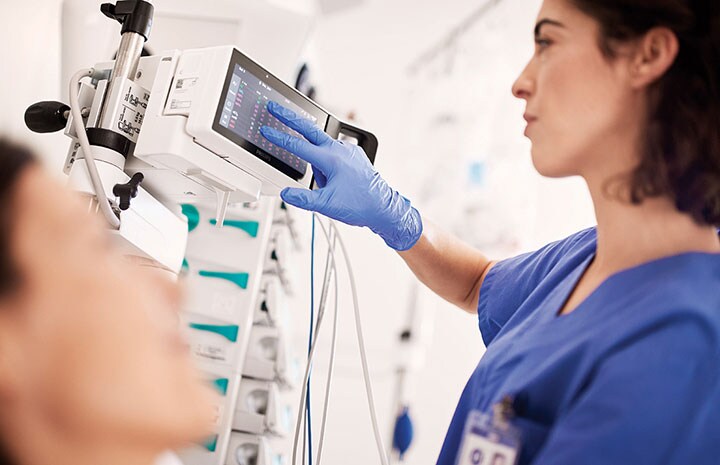
Such an “as-a-service” partnership brings together all previous tenets we discussed. It is guided by a clear shared purpose: removing technology barriers that impact patient care and staff satisfaction. It empowers the people behind the technology through ongoing training and education. And it promotes a culture of continuous optimization, using data to inform cross-functional team discussions about small workflow improvements which can ultimately have a big impact.
The most encouraging part? It works. Studies at Jackson Memorial Hospital show 13,331 in potential hours saved annually through improvements from workflow changes and automation [7], while staff satisfaction with patient monitoring systems rose from 8% to 90% [8].
Successful digital transformation puts people first
These and other examples show how real gains in digital transformation can be made in close collaboration among all stakeholders, with a strong focus on culture and change management. Together, we can reimagine how care is delivered, with healthcare professionals and patients firmly at the center – making healthcare as frictionless as any other experience.
There may not be one perfect way to get there. But one thing I do know for sure: if you want to successfully drive digital transformation, always think people first and technology second.
To learn more about how Philips is partnering with healthcare leaders on people-first digital transformation, join us virtually or in person at the upcoming ViVE and HIMSS global trade shows. You can also follow @PhilipsLiveFrom for updates from #ViVE23 and #HIMSS23.
References
[1] https://pubmed.ncbi.nlm.nih.gov/35922094/
[2] https://www.bain.com/insights/a-smarter-way-for-healthcare-companies-to-go-digital/
[3] https://eithealth.eu/wp-content/uploads/2020/03/EIT-Health-and-McKinsey_Transforming-Healthcare-with-AI.pdf
[4] https://www.philips.com/c-dam/b2bhc/global/operational-intelligence-insights/strategic-role-education-training/philips-mackenzie-integrated-file.pdf
[5] Christopher J. Kelly, Alan Karthikesalingam, Mustafa Suleyman, Greg Corrado, and Dominic King. 2019. Key challenges for delivering clinical impact with artificial intelligence. BMC Medicine 17, 1: 195.
[6] Browne, Jacob & Bakker, Saskia & Yu, Bin & Lloyd, Peter & Allouch, Somaya. (2022). Trust in Clinical AI: Expanding the Unit of Analysis. 10.3233/FAIA220192.
[7] Results from the automation of ECG wavestrip patient transport process, non-value added vitals charting, equipment upgrades, and workflow changes at Jackson Memorial Hospital. Data was collected by time study observations with the Philips team and Jackson Memorial Hospital team. These numbers are estimated projected time savings.
[8] Results from pre- and post-surveys at Jackson Memorial Hospital. Prior to the partnership with Philips, 8% of clinical teams indicated they were somewhat satisfied or highly satisfied when asked to rate their overall satisfaction with the current patient monitoring system (examples – bedside monitors, central monitoring stations, transport devices). After entering the partnership with Philips and implementing technology and workflow improvements through an as-a-service model, that number rose to 90%.
Share on social media
Topics
Author

Shez Partovi
Chief Innovation & Strategy Officer and Business Leader of Enterprise Informatics, Royal Philips Shez Partovi obtained his medical degree from the McGill University, in Montreal, Canada and completed his neuroradiology subspecialty at Barrow Neurological Institute in Phoenix, AZ. He is a serial entrepreneur and has launched several health IT companies, including two on telehealth.
Click here to read more on Shez Partovi
Follow me on