With their team having recently completed the 100th Cone Beam CT-assisted small lesion biopsy on the Azurion FlexArm at Macquarie University Hospital (MUH) on 16 April 2024, we caught up with Dr. Tajalli Saghaie, MD FRACP, Respiratory physician, Interventional pulmonologist, Associate Professor, Macquarie University, and NSW and Deputy Director of Medical Services, MUH, and Professor Alvin Ing, Respiratory Medicine Physician and Clinical Program Head of the Cardiovascular and Respiratory program at Macquarie University, to ask them 5 questions on what this means for future lung cancer patients in Australia.

1. What is Cone Beam CT bronchoscopy and what is it typically used for? Dr. Tajalli: Cone Beam Computed Tomography or CBCT is a type of advanced imaging that creates 3-dimensional pictures of the body. It can be used during surgery to help doctors get a better understanding of their patient's anatomy. While it's not commonly used by all doctors, vascular surgeons and interventional cardiologists frequently use this type of imaging in Australia and around the world. This is because it's important to have accurate imaging during surgery when dealing with the lungs, which have complicated anatomy. With CBCT, we can increase the accuracy of bronchoscopic biopsies, which can be crucial in both the diagnosis and treatment of lung cancer. 2. How has CBCT bronchoscopy on the Azurion System transformed your practice, compared to what you had available in the past? Dr. Tajalli: In the past, it has been almost impossible to biopsy small nodules in the lungs, which can be a major problem in diagnosing and treating lung cancer. Typically, doctors would take a biopsy by inserting a needle through the skin and using CT guidance. Unfortunately, this method has a poor success rate of getting a confident answer, with over 15-20% of cases experiencing complications. This not only makes it difficult to make decisions about treatment, but also leads to additional costs and health risks.
Before CBCT with the Azurion system, the best options were either for doctors to wait for cancerous lesions to grow larger before taking a biopsy, or treat them without a proper diagnosis. The former leads to considerable negative impact on overall patient outcomes in lung cancer, and the latter leads to higher costs for unnecessary treatments or procedures, and health complications in up to 10-20% of patients.
With the advent of CBCT, we can now biopsy these small nodules safely and accurately, providing crucial information for multidisciplinary lung cancer meetings to make the best decisions for our patients.
Alongside Philips as one of our close partners, we remain committed to our mission to improve lung cancer care in Australia, and to promote equity by making sure access to CBCT technology is not limited to anyone in the country.
Dr. Tajalli Saghaie
MD FRACP, Respiratory physician, Interventional pulmonologist Associate Professor, Macquarie University NSW and Deputy Director of Medical Services, MUH Organization: Macquarie University Hospital
3. Out of the 100 biopsies your team have completed, what was your most memorable patient and why? How did they benefit from the CBCT bronchoscopy procedure using the Azurion System at Macquarie University Hospital? This allowed my patient to successfully undergo minimally invasive surgery just 22 days after first being seen by myself. Ultimately, because she was diagnosed at an early stage, she was able to be cured. This patient also had a relative who was not so fortunate, as they had been diagnosed late with lung cancer symptoms – a key reason why lung cancer is the most deadliest of cancers in Australia. My patient’s successful diagnosis and treatment was largely due to the accurate and reliable imaging provided by CBCT guidance, which has expanded our ability to diagnose small peripheral lung lesions early, a crucial factor in promoting curative therapy. This case really drove home the potential of CBCT-guided bronchoscopic biopsy as a game changer in the diagnosis of early lung cancer. Dr. Tajalli: As Professor Alvin shared, one of the common scenarios where we get patients referred to us is in cases where they are told that conventional non-CBCT biopsy is not possible and not an option for them – usually because their lung nodules are too small, as I’ve previously mentioned. Other scenarios we’ve come across in referred patients is where a biopsy had already been done and failed (or been complicated), sometimes repeatedly! The constant refrain in all these cases is that CBCT bronchoscopy has successfully helped us diagnose lung cancer where traditional biopsies have failed, and that is why my team and I are very excited and eager for more doctors in Australia to learn more about it, practice it and increase patient access to it.
Professor Alvin: One of my most memorable patients was also one of my first. In May 2023, a woman of Asian background with a family history of lung cancer presented with a new 11 mm ground glass lung lesion. Traditional methods for diagnosing such small pure ground glass lesions have low success rates due to difficulty in locating them accurately. However, using the Philips Azurion CBCT, I was able to pinpoint, segment and biopsy the lesion with precision by navigating an ultrathin bronchoscope successfully to it. An on-site cytopathology test was immediately able to identify malignant cells on the smears, with final tests leading to an early diagnosis of adenocarcinoma with a specific mutation.
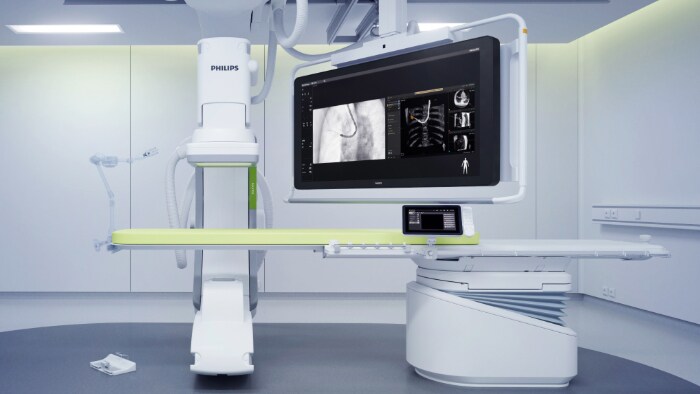
4. Why is the imaged guidance enabled by CBCT bronchoscopy such a big deal? Why should physicians and patients sit up and listen? Dr. Tajalli: When lung cancer screenings begin in earnest in Australia, we will likely be overwhelmed by a tsunami surge of small lung nodules needing to be biopsied. The point of lung cancer screening is to find lung nodules when they are small, and diagnose them early, because early detection is key to successful treatment. Lung cancer, when diagnosed early, can be curable. Without a way to safely and reliably biopsy these small lung nodules, lung cancer screening is not going to be successful in its end goal, which is to create a stage shift in lung cancer population by diagnosing and treating them early. This is where CBCT bronchoscopy comes in - it provides a safe and dependable method to biopsy small lung nodules, even if they are located in hard-to-reach spots. Ultimately, this helps to improve the speed, volume and efficacy of lung cancer interventions, enhance overall patient outcomes and population health. Professor Alvin: Agreed, CBCT in my mind has opened up our ability to accurately diagnose small peripheral lung lesions. With the imminent onset of lung cancer screening, CBCT is vital in my view to promote accurate early diagnosis and therapy of lung cancer.
My patient’s successful diagnosis and treatment was largely due to the accurate and reliable imaging provided by CBCT guidance, which has expanded our ability to diagnose small peripheral lung lesions early, a crucial factor in promoting curative therapy.
Professor Alvin Ing
Respiratory Medicine Physician and Clinical Program Head of the Cardiovascular and Respiratory program Organization: Macquarie University
5. How has Philips been partnering with your team at MUH since the start of this journey? What do you hope to achieve in future collaborations? Dr. Tajalli: After an educational trip to the US and seeing the Azurion system in action, I realized that we already have the exact same system in our theatre room at Macquarie University Hospital (MUH). After contacting the Philips team in the US and communicating with the local team in Australia, they were able to organize a trial upgrade on our system at MUH, and we successfully completed our first CBCT procedure on a patient in May 2023. • Associate Professor Jonathan Williamson, Respiratory and Sleep Physician at Macquarie University Hospital • Dr. Paul Lilburn, Respiratory Physician at Macquarie University Hospital and Prince of Wales Hospital • Dr. Samantha Herath, Respiratory Medicine & Sleep Medicine Specialist at Macquarie University Hospital • Dr. Benjamin Ng, Respiratory and Sleep Physician at Macquarie University Hospital • Clinical Professor Martin Phillips, Consultant Respiratory Physician and Honorary Clinical Professor at Macquarie University
Things moved pretty rapidly from there, and after an exciting learning curve, this has become a routine procedure for us with multiple bronchoscopists at MUH performing this confidently. It’s been a huge team effort in getting us to this significant milestone of 100 CBCT procedures completed in Australia, and along with Professor Alvin I’d also like to give credit to the fantastic contributions by the following doctors to make this possible:
I am also very happy to see that we have been able to spread our knowledge and experience with colleagues around Sydney and the rest of Australia, with other hospitals coming onboard this year. Alongside Philips as one of our close partners, we remain committed to our mission to improve lung cancer care in Australia, and to promote equity by making sure access to CBCT technology is not limited to anyone in the country.
Share on social media
Topics
Contacts

Yi Xian, Tan Brand & Communications Manager Philips Australia & New Zealand
You are about to visit a Philips global content page
Continue