The 2021 Philips Future Health Index (FHI) report explores the challenges to digital transformation faced by almost 3000 healthcare leaders around the world. Issues such as investment, interoperability and staffing are common to the New Zealand landscape, along with a drive to adopt new models of care.
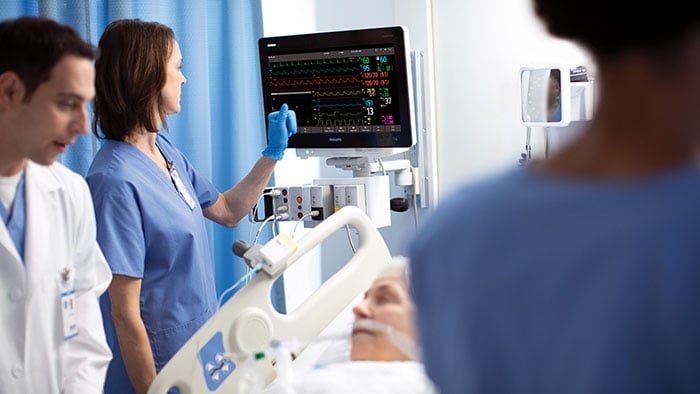
Healthcare leaders across the globe have recognised the important role digital health technology has played in tackling Covid-19 and ensuring the continued delivery of care in incredibly difficult circumstances.
New Zealand and Australia’s healthcare systems have performed well in response to the pandemic, contributing to a feeling of optimism about the future. However, there is caution about whether the rapid transformations and use of technologies will become embedded and whether the policy changes and financial incentives are in place to encourage that shift.
Going forward, we need to capitalise on the positive actions taken throughout this pandemic and nurture the additional resilience we have gained. The New Zealand and Australian experience provides significant lessons that can inform and shape our response to future global crises,”
Matt Moran
Managing Director of Philips in Australia and New Zealand
The need for interoperability A lack of interoperability or data standards across systems is cited by healthcare leaders as the top barrier to the adoption of digital health technologies within their healthcare facilities, according to the 2021 Future Health Index report. Matt Moran says New Zealand’s plans for a national Health Information Platform, called Hira, will help address this problem locally. “With a platform for interoperability, everyone has access to the same data and can use that to inform decisions and get better outcomes,” he says. “That will also address some of the geographic disparities and health inequities in New Zealand.” Shehaan Fernando, Philips Regional Director Care, explains that patient care is compromised if data does not flow easily between the many services consumers interact with as they journey through the health system. The 2021 FHI report says a lack of interoperability across platforms is also frequently cited as a pain point for healthcare professionals and could be contributing to a perception of staff resistance to using more advanced technologies. The importance of partnerships The 2021 FHI report reveals that 35% of Australian healthcare leaders are looking to prioritize strategic partnerships and collaborations to successfully implement digital health technologies. Of those healthcare leaders, 45% see partnerships with Health Informatics companies as a necessary step to help drive their digital transformation agenda. Globally, healthcare leaders reported their staff’s lack of experience with new technology as the top internal barrier to preparing for the future. Moran says although healthcare leaders are struggling with staff shortages, a challenge exacerbated by border closures in both Australia and New Zealand during the pandemic, collaborating with industry players is an opportunity to bridge the gap. “It’s important to invest in nurturing a local talent pipeline and there's certainly a role within the education system to make sure, whatever the sector, that people going into the workforce are digitally capable, as that can drive productivity of the entire economy.” The recently published New Zealand Health IT (NZHIT) Report reveals that our health workforce’s overall level of digital literacy needs to be improved to fully utilize and benefit from the implementation of digital health technologies. In the 2020 Future Health Index report, roughly half (47%) of younger Australian healthcare professionals indicated they didn’t know how to use digital patient data to inform care. However, in the 2021 FHI report, staff training is cited by only around one-third of Australian healthcare leaders as an action that their hospital or healthcare facility needs to take to successfully implement digital health technologies. Philips welcomes the New Zealand government’s investment in telehealth projects via its Digital Enablement Fund as their research shows investment is needed to incentivise people to change their ways of working. Budgets as a barrier Around the world, limited budgets are also cited as a key barrier to technology adoption. Moran says the upfront costs of investing in new technologies have been prohibitive in the past, but the expansion of the Cloud, and ‘healthcare as a service’ or subscription models, have changed the equation. “Technology has evolved to be more decentralised, independent and Cloud-based and that helps alleviate some of the challenges,” he explains Investment in digital solutions can also provide a return on investment by keeping people out of hospital, as well as improving their quality of care. “Part of our job is to make sure that the data and the benefits are clear, in order to drive some of those more difficult short-term decisions for the longer term sustainability of the system.” Adding “the budget allocated by the New Zealand government for the digital transformation of industry reflects the growing demand of the healthcare sector for e-health services. We’re excited to see how the increased digital-first focus from the government will impact the healthcare space and the opportunities that this could open up.” Care closer to home Health Minister Andrew Little recently announced sweeping reform of New Zealand’s health system, with a focus on delivering services closer to home, using digital options. This shift towards more care in the community aligns with an international trend identified in the 2021 FHI report. In the future, Australian healthcare leaders anticipate, on average, that roughly a quarter of routine care delivery will take place outside the walls of their hospital or healthcare facility. Philips is running a virtual care program in Queensland where cardiac patients are monitored at home and an economic impact assessment commissioned by the Australian Centre for Health Services Innovation (AusSHI) shows a 30 percent drop in hospital readmissions. This involves patients being cared for in the community, with the use of remote monitoring and coaching to support them to improve their health and wellbeing. Fernando says while telehealth has its place, the real opportunity to transform care is moving towards a more comprehensive virtual healthcare system. Not only does this approach make the system more sustainable, it is also what patients and health professionals want and expect, he says. The local landscape The FHI report reveals a range of challenges to digital transformation of the health system, which all need to be addressed in order to drive the agenda forward. Recent history has shown us how important it is to have a robust digital health strategy in place that allows care to be delivered outside the hospital. Evolving models of care and addressing health disparities for our most vulnerable populations, will demonstrate our ability to harness lessons learnt and contribute to building a resilient healthcare system. This interview was originally published in the July edition of Digital Health Connect Magazine
“This kind of collaboration on digital transformation needs to become the top priority for tech companies, major businesses and governments alike if New Zealand is to remain an innovative, competitive player in a digital world,” he says.