West Moreton Hospital and Health Service and Philips launch MeCare, a personalised connected health management program for high needs patients in Australian communities
Revolutionary population health management model of care offers independence to patients who suffer complex chronic illness
October 27, 2016
Brisbane, Australia – Royal Philips (NYSE: PHG, AEX: PHI) together with West Moreton Hospital and Health Service (WMHHS) and Queensland Health have launched a connected health program using the latest health data technologies. The program, called MeCare, will deliver proactive, continuous and integrated patient care for Australians with complex chronic illness who consequently have reduced quality of life and require frequent hospitalisations. This is the first program in Australia and Asia Pacific helping the high acuity complex chronic population. MeCare aims to improve the health and quality of life for individuals from the West Moreton community with chronically poor health, while providing significant economic benefits also to the hospital and health system. The program is tackling the challenges of increased expectations to improve self-management, to be treated closer to home, of an ageing population and of increased pressure on the hospital system, by transforming the delivery of care supported by connected health technology. MeCare is highly personalised with health management plans specifically tailored to each patient’s current behaviours. A patient receives the Philips eCareCompanion, an easy-to-use telehealth app that patients access on a secure tablet at home, and a range of monitoring devices such as a blood pressure monitor, a pulse oximeter and a weight scale. With just a few simple steps, a patient’s vital information is captured wirelessly and transmitted to their care team for review. They can also answer survey questions, receive reminders about their care plan and connect to their care team via a video call. With this program in place, the West Moreton and extended community is able to make more timely care decisions and intervene earlier, leading to fewer hospitalisations and enhanced patient self-care. The participants will be cared for in the community most of the time by a multi-disciplinary team that includes their family/carer, GP, specialists, allied health professionals and social and community support services; therewith reducing their reliance on hospital inpatient and emergency services.
Kevin Barrow, Managing Director Philips Australia and New Zealand, said the MeCare program is a new value-based care approach to delivering what is often challenging and expensive levels of care. “We are very excited to be able to deploy this solution in Australia and improve not only the lives of patients with chronically ill health, but with that bring the ability to embed and connect care across the entire health systems enterprise to treat as many high needs patients as possible. “Historically the provision of care for the chronically ill has been resource heavy and inefficiently managed. With this solution from Philips and holistic community care from hospitals like West Moreton HHS, who are bold enough to try innovative solutions, we are able to demonstrate reduced reliance on hospital-based inpatient, outpatient and emergency services when it comes to chronic care; improving operational efficiency and sustainability while providing cost savings,” said Barrow. West Moreton Hospital and Health Service Chief Executive Sue McKee said the hospital is incredibly excited about the potential of this technology to shift current chronic disease management to a more sustainable model of care. “The relatively small number of patients that suffer chronic diseases often take a disproportionate amount of funding, and while necessary, this is ultimately unsustainable long-term. The potential in the MeCare model to not only change that, but improve patient outcomes could have pronounced implications industry-wide.” The WMHHS MeCare Program is underpinned by the Philips’ market-leading population health management solution, Integrated Tailored Ambulatory Care (ITAC). The solution runs on Philips’ enterprise telehealth platform eCareCoordinator, which is built on the Philips HealthSuite digital platform, a secured cloud-based platform of services, capabilities and tools used to create the next generation of connected health and wellness innovations. The platform has clinical decision support tooling and incorporates deterioration algorithms to predict patient deterioration. The eCareCoordinator platform prioritises populations so clinicians can identify and provide care to the patients most at risk for readmission, provides structure for cross-team collaboration and delivers extended reporting so program effectiveness can be measured and continuously improved. Successful ambulatory care programs in Banner Health (US) and Liverpool (UK) that Philips has trialled have demonstrated that for chronic patients with more complex health needs than is anticipated for this service, a reduction in chronic disease related resource utilisation and cost in inpatient, emergency department and services can be achieved by approximately 45%[1]; and a 20% to 30% net reduction in cost of care[2][3] is achievable. These results show that significant health economic benefits including improved patient satisfaction, reduction in hospitalisation and emergency department presentations, and reduced acute and long-term care costs and improved health outcomes can be realised. [1] https://www.usa.philips.com/a-w/government/articles/Banner-Health-achieves-cost-of-care-savings-with-telehealth.html [2] https://www.philips.co.uk/a-w/about/news/archive/standard/news/press/2016/20160527-philips-results-three-year-telehealth-study.html
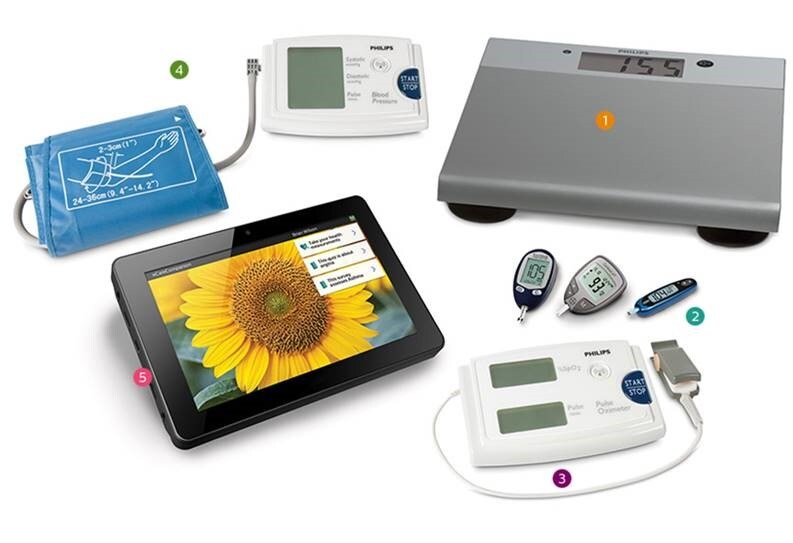
The MeCare solution suite featuring Philips eCareCompanion
For further information, please contact:
Albertine Schor Brand Communications Manager Philips Australia and New Zealand Mob: +61 427 915 643 Email: albertine.schor@philips.com West Moreton Hospital and Health Service
Corporate Communications
Phone: 07 3413 7922
Email: wmcommunications@health.qld.gov.au
About Royal Philips
Royal Philips (NYSE: PHG, AEX: PHIA) is a leading health technology company focused on improving people’s health and enabling better outcomes across the health continuum from healthy living and prevention, to diagnosis, treatment and home care. The Company leverages advanced technology and deep clinical and consumer insights to deliver integrated solutions. The Company, headquartered in the Netherlands, is a leader in diagnostic imaging, image-guided therapy, patient monitoring and health informatics, as well as in consumer health and home care. The Company’s health technology portfolio generated 2015 sales of EUR 16.8 billion and employs approximately 69,000 employees with sales and services
in more than 100 countries. News about the Company can be found at www.philips.com/newscenter.

